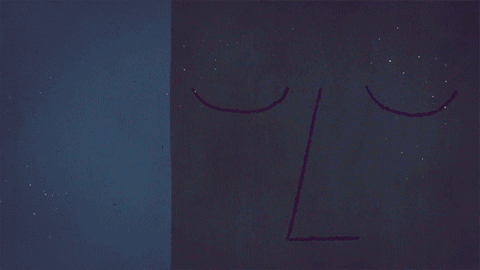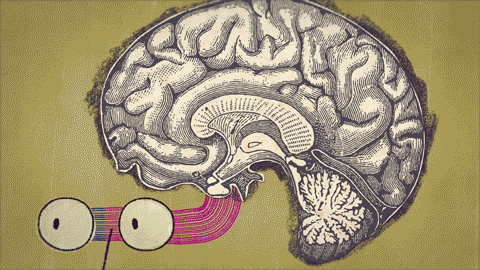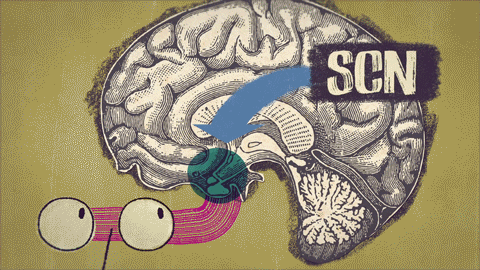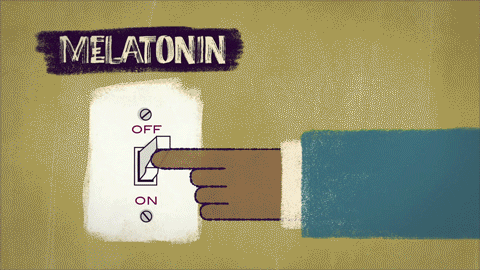The Light that Makes the Differnce
NoLight-ICU, Light for the ICU Patient
Published
Acute brain dysfunction frequently accompanies critical illness. Delirium is the most common manifestation of ABD in the intensive care unit and is independently associated with higher 6-month mortality and long-term cognitive impairment. It defines an acute disturbance of attention, awareness, and cognition, which typically fluctuates during the day. The fluctuating nature of delirium indicates its link to the circadian system.
The master clock, located in the hypothalamic suprachiasmatic nucleus (SCN), generates the circadian rhythm. Efferent signals from the SCN regulate the secretion of melatonin produced by the pineal gland. Light received by the photoreceptors in the retina is the most important stimulus for steering circadian rhythmicity in humans.
Daylight uses the polysynaptic intrinsically photosensitive retinal ganglion cells- (ipRGCs) signalling pathway of ’non-visual’ circadian photoentrainment to synchronise our endogenous oscillator to the 24-hour day. The observed suppression of pineal melatonin production in response to a sufficient light exposure requires the eyes to be open so that the retinal photoreceptors can process the stimulus.
Sleeplessness during critical illness is one of the most frequent stressors reported by ICU survivors. In fact, several studies reported abnormalities of sleep quantity and quality with a significant decrease in slow wave sleep (SWS) and rapid eye movement (REM) sleep. In addition, several studies revealed that critically ill patients suffer from alterations in their circadian rhythm of melatonin production.
As a consequence of these findings, using light to maintain or entrain circadian rhythm seems the optimal intervention that might have a much better risk-benefit ratio than those used in clinical routine today.
Guidelines for ICU design recommend a daylight source for every patient room. and artificial light that can be dialed up and down to minimize circadian rhythm disruptions.
But what makes a light source adequate in supporting circadian rhythmicity of a critically ill patient?Our working group has just evaluated photometric parameters of three different electric light sources in the ICU, including the newly developed, 15 square meters large LED light-ceiling. Furthermore, we aimed at estimating potential circadian efficacy and side effects of the light sources for exposed patients.